After years of debilitating seizures, unexplained falls, and being told by doctors she was simply “anxious” or “depressed,” a 23‑year‑old Welsh woman turned to ChatGPT in a last‑ditch plea for answers. The AI chatbot not only listened — it delivered a correct diagnosis in minutes, a rare genetic condition that had eluded the medical system for over a decade.
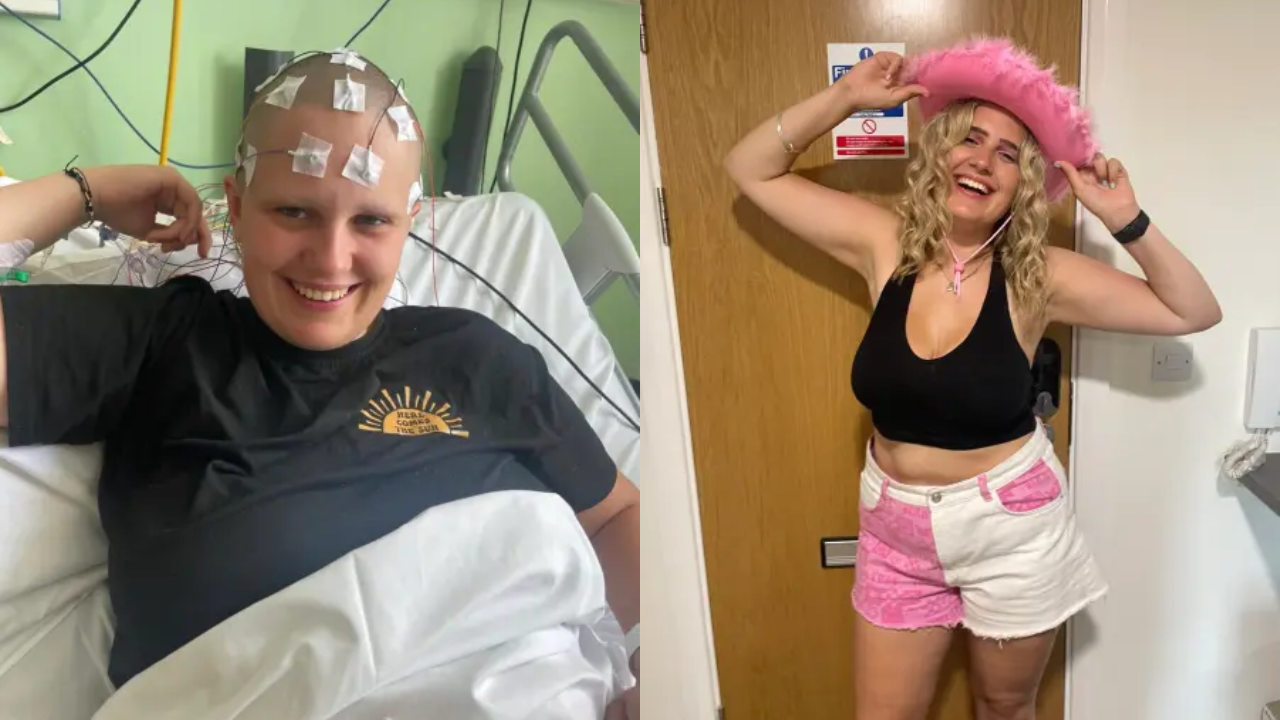
Phoebe Tesoriere, from Cardiff, Wales, had been suffering from seizures, falls, balance problems, and a progressive loss of mobility since childhood. She was misdiagnosed with anxiety, depression, and epilepsy, and claims she was warned that she would be treated as a mental health patient if she kept returning to the emergency room.
Desperate, lonely, and exhausted, she typed her symptoms into ChatGPT. The AI suggested hereditary spastic paraplegia (HSP), a rare genetic neurological disorder. She brought the finding to her doctors, who ordered genetic testing — and confirmed the AI was right.
“I had no history of anxiety. I was a really happy, bubbly person,” Tesoriere told the BBC. “To be told it was all in my head was devastating.”
A Lifetime of Mystery: From Childhood Limp to Seizures
Tesoriere’s medical odyssey began in childhood. She was born without a hip socket and underwent operations as a baby, leaving her with a limp that doctors initially attributed to her early surgeries. She was later tested for dyspraxia, a coordination disorder, but the results were negative.
At 19, she collapsed from her first seizure. Doctors attributed it to anxiety, but Tesoriere was unconvinced. “I had no history of anxiety,” she said. By 2022, she was diagnosed with epilepsy and put on medication. Instead of improving, her symptoms worsened. She struggled to walk, suffered more frequent seizures, and was later diagnosed with Todd’s paralysis, a temporary post‑seizure condition that can mimic a stroke.
In January 2025, she fell down a flight of stairs and spent three months in the hospital undergoing a barrage of tests — all inconclusive. Seven months later, a severe seizure left her in a coma for three days. When she woke, doctors again told her it was anxiety.
“It was really, really lonely,” she told the BBC. “I had no idea what was happening to my body.”
‘I Was Desperate’: How ChatGPT Cracked the Case
Feeling dismissed and hopeless, Tesoriere turned to ChatGPT. She fed the AI her symptoms, medical history, and the results of previous tests. Within minutes, the chatbot suggested she might have hereditary spastic paraplegia (HSP) – a rare genetic condition characterized by progressive muscle stiffness and weakness in the legs.
She took the AI’s suggestion to her doctors. This time, they listened. Genetic testing was ordered, and the results confirmed what ChatGPT had proposed.
“The fact that a free online tool could figure it out in minutes, when doctors had been scratching their heads for years, is both amazing and terrifying,” Tesoriere said.
A spokesperson for the Cardiff and Vale Health Board, the regional NHS authority responsible for her care, said in a statement: “We are sorry to hear about Phoebe’s experience while in our care.”
Understanding Hereditary Spastic Paraplegia (HSP)
Hereditary spastic paraplegia is not a single disease but a group of more than 80 inherited neurological disorders. Its hallmark symptom is progressive stiffness and weakness in the legs, caused by degeneration of the long nerve fibers that control movement.
| Key Facts About HSP |
|---|
| Prevalence: Estimated 1–10 cases per 100,000 people globally |
| Typical onset: Any age, but often begins with a subtle gait disturbance in childhood or early adulthood |
| Primary symptoms: Lower‑extremity weakness, muscle tightness (spasticity), impaired balance, and difficulty walking |
| Progression: Gradual; many patients eventually require a wheelchair |
| Diagnosis: Clinical exam, family history, and genetic testing |
| Treatment: No cure; symptoms managed with physical therapy, muscle relaxants, and assistive devices |
The disease is considered “rare” by medical standards, and its symptoms often mimic those of more common conditions like multiple sclerosis, cerebral palsy, or even anxiety disorders — contributing to frequent misdiagnosis.
“HSP is a great mimicker,” said Dr. Helen Matthews, a consultant neurologist at the University of Cardiff. “It’s not on every doctor’s radar, and patients can spend years bouncing between specialists before someone thinks to order genetic testing.”
The AI Diagnosis Revolution: Promise and Peril
Tesoriere’s case is not an isolated incident. Across the globe, patients are increasingly turning to AI chatbots for diagnostic help — with remarkable, and sometimes unsettling, results.
| Notable AI Diagnosis Cases | Outcome |
|---|---|
| US patient, 10+ years of mystery symptoms | ChatGPT identified MTHFR gene mutation; doctors confirmed |
| 17‑year‑old UK boy, misdiagnosed with Raynaud’s syndrome | ChatGPT identified rare neurological disorder; hospital confirmed |
| 40‑year‑old woman, dismissed by multiple doctors | ChatGPT flagged Hashimoto’s disease; tests confirmed thyroid cancer |
Research has begun to quantify AI’s diagnostic potential. A 2024 study in Nature found that ChatGPT‑4 solved all common medical cases within two diagnostic suggestions. For rare diseases, it needed eight or more suggestions to reach 90% accuracy — far from perfect, but still outperforming many general practitioners on pattern recognition.
A separate study in Annals of the Rheumatic Diseases reported that ChatGPT correctly diagnosed rare rheumatologic conditions in 83% of test vignettes, often in under one minute.
However, experts caution that AI is not a replacement for medical training. The same studies note that AI can produce “medically implausible” reasoning, miss subtle symptoms, and cannot replace the nuance of a physical examination.
“AI is an incredible tool for generating differential diagnoses, especially when a patient has a long, complicated history,” said Dr. James Turner, a digital health researcher at Oxford. “But it’s still a tool. The final diagnosis must come from a human doctor.”
A Broken System: The Reality of Rare Disease Diagnosis
Tesoriere’s story also highlights a systemic failure. According to a 2025 report from the UK’s Independent newspaper, the National Health Service (NHS) is “not working” for people with rare diseases, with nearly 30% of patients waiting five years or more for an accurate diagnosis. The report estimated that 3.5 million people in the UK live with a rare disease, many of whom face long diagnostic delays.
In some cases, the consequences are fatal. A coroner recently warned that a lack of national guidance on diagnosing a rare brain disorder could lead to further deaths after a 12‑year‑old girl with undiagnosed autoimmune encephalitis took her own life while sectioned in an NHS psychiatric unit.
“The system is not designed for rare diseases,” said Dr. Matthews. “Doctors are trained to look for horses, not zebras. Patients like Phoebe are the zebras, and the system needs to get better at finding them.”
Tesoriere is now in a wheelchair, managing her symptoms through physical therapy. She can no longer work as a teacher, but she is pursuing a master’s degree in psychology.
“I want to do something that helps people,” she said. “No one should have to go through what I went through.”
What’s Next for Phoebe and for AI in Medicine?
- Ongoing management: Tesoriere will continue physical therapy and symptomatic treatment. There is no cure for HSP, but early diagnosis allows for better long‑term planning.
- NHS review: The Cardiff and Vale Health Board’s apology may signal internal reviews, but systemic changes to rare‑disease diagnosis are still lacking.
- AI integration: Hospitals are beginning to pilot AI diagnostic support tools, but widespread adoption remains years away.
- Patient empowerment: Cases like Tesoriere’s are fueling a new wave of “patient‑led diagnosis,” where individuals use AI to advocate for themselves within the medical system.
FAQ: ChatGPT and Rare Disease Diagnosis
Q: What is hereditary spastic paraplegia (HSP)?
A: A group of rare genetic disorders that cause progressive stiffness and weakness in the legs. It is often misdiagnosed as cerebral palsy, multiple sclerosis, or even anxiety.
Q: Is ChatGPT a reliable diagnostic tool?
A: Studies show it can be highly accurate for common conditions and surprisingly good at generating plausible diagnoses for rare diseases. However, it can also make errors and should never replace a doctor’s clinical judgment.
Q: Why did doctors miss the diagnosis for so long?
A: HSP is rare, its symptoms overlap with more common conditions, and general practitioners may not have it on their mental “differential diagnosis” list. Tesoriere was also young and female, a demographic whose physical symptoms are historically more likely to be dismissed as psychological.
Q: Can I use ChatGPT to diagnose myself?
A: You can use it to generate ideas to discuss with your doctor, as Tesoriere did. But you should never rely on it as a definitive diagnosis.
Q: Where can I learn more about HSP?
A: The National Organization for Rare Disorders (NORD) and the Spastic Paraplegia Foundation are excellent resources.